Restorative Dentistry, Implant Dentistry
Dental Implant Problems, Risks, and Timeline: What Patients in Bellflower Need to Know
Dental implants succeed at a high rate, but the real problems patients face go beyond whether the implant fuses to the bone — they include sensory changes, mechanical maintenance, and a timeline that varies based on surgical decisions made before the first incision. Understanding these realities upfront leads to better outcomes and fewer surprises.
The Sensory Problem Nobody Warns You About
Most people expect a dental implant to feel exactly like the tooth they lost. For Bellflower-area patients, this expectation sets up the most common disappointment I see in my practice.
Your natural teeth aren't anchored rigidly to bone. They're suspended by the periodontal ligament — a thin, nerve-rich tissue that acts as a biological shock absorber. That ligament gives your tooth a tiny amount of "give" and, more importantly, sends pressure signals to your brain. This is called proprioception, and it tells you how hard you're biting before you go too far.
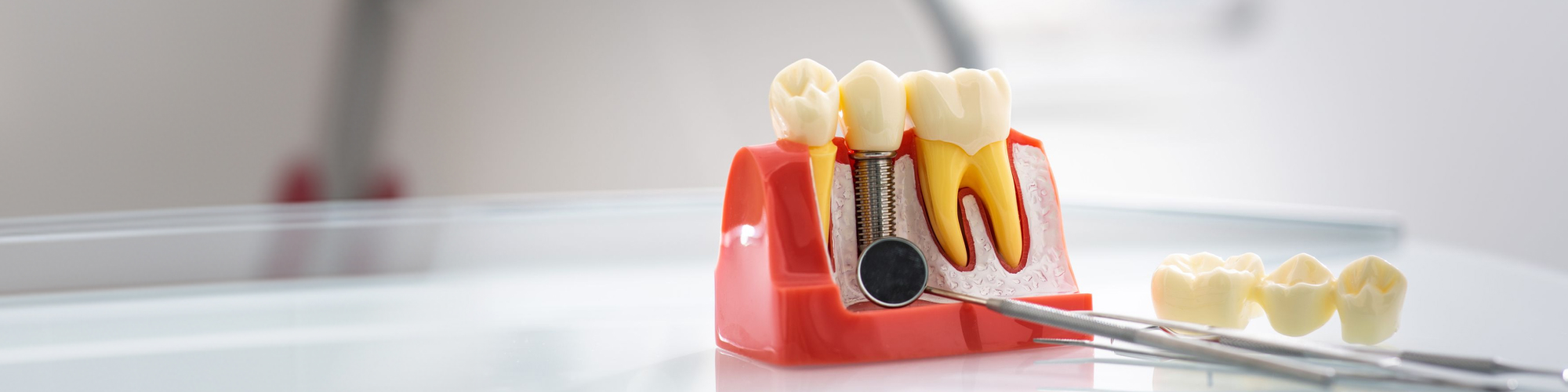
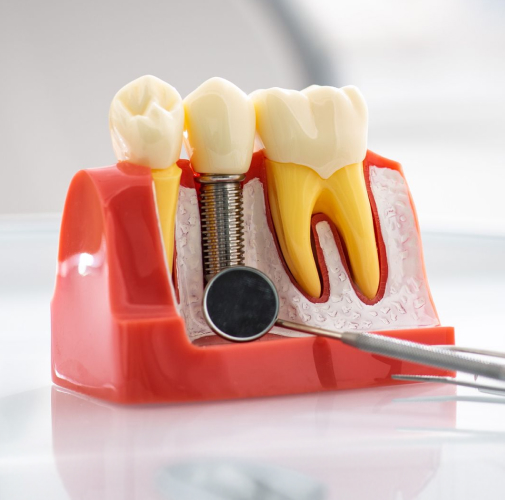
Implants have no periodontal ligament. The titanium post fuses directly to your jawbone through osseointegration. That's what makes implants so stable — but it also means the sensory feedback disappears. The implant itself feels "dead" compared to a natural tooth.
Clinically, this matters. Without that feedback, patients commonly bite down harder than they intend on the opposing teeth. Over time, this can contribute to chipping of adjacent teeth or jaw fatigue, especially in people who already grind. According to Mayo Clinic, nerve damage and surrounding structural issues are recognized surgical risks — but the subtler loss of bite proprioception is a daily functional reality that begins the moment osseointegration is complete.
The adjustment period is real. I tell patients to expect a relearning phase of several weeks where they consciously moderate bite force. Softer foods early on aren't just about protecting healing bone — they help the brain recalibrate to a new mechanical reality. Most people adapt fully, but knowing this in advance prevents panic when the implant feels different than expected.
Screw Loosening vs. Implant Failure: The 10-Year Maintenance Reality
Here's what most implant articles skip entirely: the implant body in your jawbone is designed to be permanent. The hardware connecting your crown to that implant is not.
Inside every implant system, a tiny abutment screw holds the crown in place. This screw is subjected to occlusal forces every time you chew — thousands of cycles per day. Research published in PMC identifies metal fatigue from biomechanical overloading as the most frequent cause of late implant-related mechanical failure, and connection-related problems like screw loosening increase from roughly 4% at five years to over 26% at ten years.
That distinction matters enormously for patient expectations. A loose crown or a clicking sensation doesn't necessarily mean your implant has failed. It often means the abutment screw needs tightening or replacement — a straightforward in-office procedure.
A realistic 10-year maintenance roadmap looks like this:
- Years 1–3: Osseointegration and tooth crown seating; periodic bite checks
- Years 3–7: Monitor for screw loosening; professional cleanings critical to prevent peri-implantitis
- Years 7–10+: Crown replacement may be needed due to wear; abutment screw evaluation
Healthline notes that an estimated 5 to 10 percent of implants fail — but this figure blends true osseointegration failure with mechanical complications that are far more manageable. Knowing the difference protects you from unnecessary anxiety and helps you ask the right questions at every follow-up visit.
The Surgical Decision That Shapes Your Entire Timeline
Most implant timelines you read online say "three to six months." That's accurate in the same way "a road trip takes a few hours" is accurate — it depends entirely on choices made before you leave.
The most important surgical decision affecting your daily life during healing is whether your surgeon uses a one-stage or two-stage protocol.
In a two-stage approach, the implant is placed and the gum is stitched completely over it. The implant heals under the gumline for three to six months, protected from chewing forces. A second minor procedure then reopens the gum to attach a healing abutment. This is the more conservative approach and is often preferred when bone quality is marginal or bone grafting was involved.
In a one-stage approach, a healing abutment — a small metal nub — protrudes through the gum immediately after implant placement. There's no second surgery, saving both time and recovery. The tradeoff is that the healing abutment is exposed to the oral environment, and patients must be careful not to accidentally load the implant with biting forces too early.
Cleveland Clinic explains that osseointegration alone takes three to nine months depending on individual healing. Add pre-surgical bone grafting — which can require its own three-to-twelve-month healing window — and some patients are looking at a 12-to-18-month total process.
Before your surgery, ask your surgeon directly: Are we doing one-stage or two-stage? Do I need a bone graft first? Those two answers will define your actual calendar far more precisely than any general estimate.
Medical Risks Worth Knowing Before You Commit
Beyond the mechanical realities, certain biological factors meaningfully increase implant risk and deserve honest discussion.
Smoking is the most significant modifiable risk factor. A WebMD overview identifies gum disease — infection and inflammation around the implant — as a primary pathway to failure, and smoking dramatically accelerates that process by restricting blood flow and impairing healing. Failure rates for smokers can reach 20 percent compared to roughly 5 percent for nonsmokers.
Uncontrolled diabetes slows the osseointegration process. Autoimmune conditions and certain medications — including proton pump inhibitors, antidepressants, and bisphosphonates — can interfere with bone metabolism in ways that compromise how well the implant fuses. Harvard Health specifically lists bisphosphonate use and chemotherapy as conditions that may disqualify a patient from implant candidacy altogether.
At our practice, we conduct thorough medical history reviews precisely because these factors don't disqualify most patients outright — they require a modified protocol. Bone grafting, staged loading, or adjusted healing timelines can bring many medically complex patients to a successful outcome. The key is identifying risks before surgery, not after. Patients who maintain regular cleaning and exam appointments give our team the best opportunity to catch and address emerging complications early.
Ready to Talk Through Your Specific Situation?
Implants are one of the most reliable tooth replacement options available, but they work best when patients enter the process with accurate expectations. If you're in Bellflower or the surrounding Southeast Los Angeles area and want a candid evaluation of whether implants make sense for you — including a review of your bone volume, medical history, and the surgical protocol that fits your situation — our team is here.
Bellflower Dental Group offers multi-specialty implant care with hospital-grade oral surgery and full sedation options, all under one roof. Schedule a consultation and get real answers before you commit.
Medical disclaimer: This article is for informational purposes only and does not constitute professional dental or medical advice. Individual results vary. Consult a licensed dental professional to evaluate your specific clinical situation before making any treatment decisions.