Emergency Dentistry
Understanding Gum Infections: Symptoms, Treatment, and Healing Time
Gum infections, also known as periodontal disease, are not only painful but can lead to serious dental issues if left untreated. Recognizing the signs early and seeking prompt treatment is crucial. In this blog, we’ll explore how to identify a gum infection, effective treatment methods, and the expected healing time.
How Do You Know If You Have an Infection in Your Gums?
Identifying a gum infection early can prevent further complications. Here are common signs to look out for:
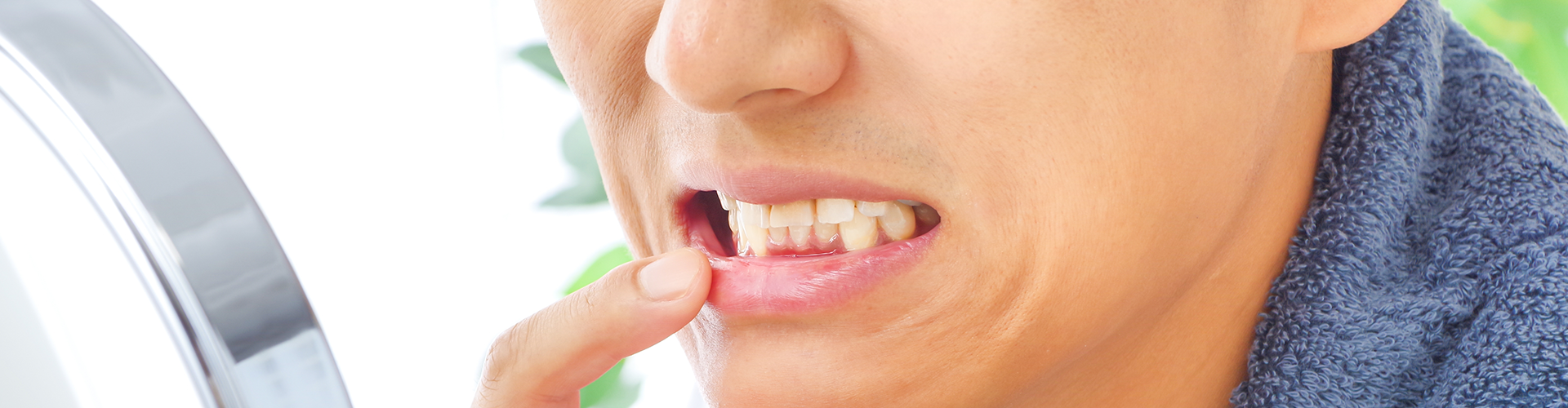
Red, Swollen Gums: Healthy gums are pink and firm, indicating good oral health. However, when your gums become red and swollen, it's a sign that your body is fighting off an infection. This inflammation is your immune system's response to bacterial invasion. It’s important to take note of any changes in the color or texture of your gums, as this can be one of the earliest indicators of a problem.
Bleeding Gums: Gums that bleed easily, especially during brushing or flossing, are often a sign of an infection. This bleeding occurs because the gum tissues are inflamed and weakened by the bacteria present. If you notice blood on your toothbrush or in the sink, don’t ignore it. It’s not just a sign of overzealous brushing—it could be a warning sign of gingivitis or periodontitis, which are stages of gum disease.
Persistent Bad Breath: Everyone experiences bad breath occasionally, but chronic bad breath that doesn’t go away after brushing or using mouthwash can indicate a gum infection. This condition, known as halitosis, is caused by the bacteria that thrive in the mouth, particularly in pockets formed by receding gums. These bacteria produce sulfur compounds, leading to a persistent bad odor.
Receding Gums: Gum recession is a process where the margin of the gum tissue that surrounds the teeth wears away, exposing more of the tooth or its root. This can be a gradual process and may not be noticeable at first. However, if you start to see more of your teeth or if your teeth appear longer, it might be due to receding gums, a common sign of a progressing gum infection.
Pain and Discomfort: Painful gums are another clear indicator of infection. This discomfort can range from a mild irritation to severe pain, especially when eating or brushing your teeth. The pain may also be accompanied by a throbbing sensation or sensitivity to hot and cold temperatures. This is your body's way of signaling that something is wrong and needs to be addressed.
Pus Formation: The presence of pus between the teeth and gums is a clear and severe sign of infection. Pus is a thick fluid produced as a result of the body’s immune response to infection. This condition, known as a periodontal abscess, requires immediate dental attention. Pus formation indicates that the infection has advanced to a serious stage and needs professional treatment to prevent further complications.
Other Symptoms: In addition to the above symptoms, some people might experience other signs of infection such as loose teeth, changes in the way your teeth fit together when you bite, or even a change in the fit of partial dentures. If you experience any of these symptoms, it is crucial to consult with a dental professional as soon as possible to prevent the infection from spreading or causing more severe damage.
Understanding these symptoms can help you take prompt action to address a gum infection. Early detection and treatment are key to preventing the progression of periodontal disease, ensuring your gums and teeth remain healthy. If you notice any of these signs, it's important to seek professional dental care immediately.
How Do You Get Rid of an Infection in Your Gums?
Treating a gum infection promptly can save your teeth and gums from severe damage. Here are the most effective treatments:
Professional Cleaning: One of the first steps in treating a gum infection is a thorough professional cleaning by a dental hygienist. This process, known as scaling and root planing, involves removing plaque and tartar from your teeth and beneath your gums. By eliminating these deposits, the cleaning helps reduce inflammation and allows your gums to heal. This procedure may need to be repeated periodically to maintain gum health.
Medications: In some cases, professional cleaning alone may not be enough to combat a gum infection, and medications may be required. Antibiotics are often prescribed to help control bacterial infection and prevent it from spreading. These antibiotics can be topical, applied directly to the affected area in the form of gels or strips, or oral, taken in pill or liquid form. Additionally, antimicrobial mouth rinses can be used to help reduce bacteria in your mouth. It’s essential to follow your dentist's instructions when using these medications to ensure their effectiveness.
Surgical Treatments: For more severe cases of gum infection, surgical treatments may be necessary to treat advanced periodontal disease. Options include flap surgery, where gums are lifted back to remove tartar and smooth damaged bone surfaces before being sutured back into place, and bone and tissue grafts, which replace lost bone or reinforce thin gums using bone fragments or soft tissue from other sources. These surgical treatments effectively reduce pockets where bacteria can hide, making it easier to keep your gums clean and healthy.
Home Care: Maintaining good oral hygiene is crucial in both preventing and treating gum infections. Consistent home care, including brushing twice a day with a soft-bristled toothbrush and fluoride toothpaste, flossing daily to remove food particles and plaque from hard-to-reach areas, and using an antiseptic mouthwash to kill bacteria and reduce inflammation, helps keep bacterial levels under control and supports the healing process.
Healthy Diet: A balanced diet rich in vitamins and minerals plays a vital role in maintaining gum health. Certain nutrients are particularly beneficial for your gums. Eating a diet that supports your overall health can also contribute to healthier gums and a stronger immune system, aiding in the fight against infections.
Regular Dental Visits: In addition to the above measures, regular dental check-ups are vital for preventing and managing gum infections. Your dentist can monitor your gum health, provide professional cleanings, and catch early signs of infection before they become serious. Don’t wait for symptoms to appear—schedule regular visits to maintain optimal oral health.
How Long Does It Take for a Gum Infection to Heal?
The healing time for a gum infection depends on the severity of the infection and the treatment method.
Mild Infections: With proper home care and professional cleaning, mild infections can start to heal within a week.
Moderate Infections: Antibiotic treatment and deep cleaning may take two to three weeks for noticeable improvement.
Severe Infections: Surgical treatments might require several weeks to months for full recovery.
Regardless of the severity, follow-up visits are essential to ensure the infection is fully resolved and to prevent recurrence.
Conclusion: Don’t Delay—Schedule Your Appointment Today!
Gum infections can escalate quickly, leading to more serious dental problems. If you’re experiencing any symptoms of a gum infection, don’t wait. Schedule an appointment with our experienced dental team today. We’re here to provide you with comprehensive care and help you maintain a healthy, beautiful smile.