Emergency Dentistry
Understanding Periodontal Disease
Periodontal disease, commonly known as gum disease, is more than just an oral health issue—it's a condition that can impact your overall well-being. As a dental office committed to your health, we've compiled a list of frequently asked questions to help you understand and manage periodontal disease effectively.
What is the First Stage of Periodontal Disease?
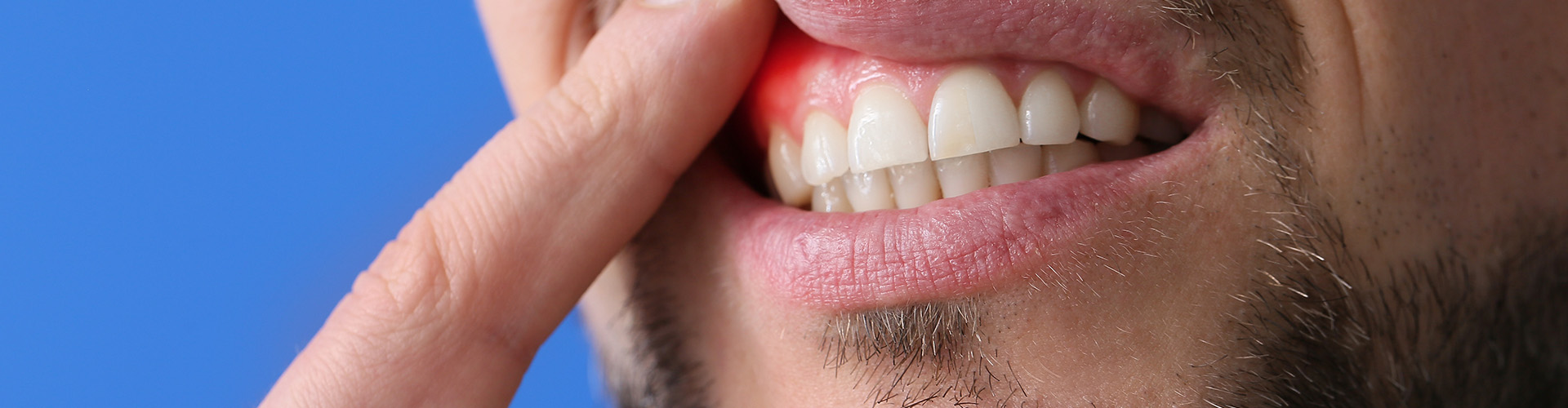
The first stage of periodontal disease is gingivitis, marking the beginning of gum-related issues that can escalate if not promptly addressed. During this phase, patients often notice their gums becoming red, swollen, and tender, a direct response to plaque accumulation at the gumline. This discomfort is most apparent during routine oral hygiene practices, such as brushing and flossing, where bleeding might occur.
Gingivitis arises from the unchecked buildup of plaque, a sticky and colorless film teeming with bacteria. These bacteria produce toxins that irritate the gum tissue, leading to inflammation. Daily activities, such as eating and brushing, can contribute to plaque formation. However, with regular and thorough oral hygiene, plaque can generally be controlled and removed.
If plaque remains on the teeth for an extended period, it can calcify into tartar (or calculus), a hard substance that adheres strongly to tooth surfaces, particularly below the gumline. Tartar is much more difficult to remove than plaque and requires professional dental cleaning to eliminate. Its presence further irritates the gums, creating a more conducive environment for bacteria to thrive and infect.
The progression from gingivitis to more severe forms of periodontal disease typically involves the transition from a reversible condition to one that can cause irreversible dental damage. However, the good news is that gingivitis is preventable and reversible with diligent oral hygiene and regular professional care. Effective brushing and flossing, coupled with professional dental cleanings, can usually reverse the effects of gingivitis. By disrupting the plaque's ability to bind to the teeth, these practices are fundamental in preventing the progression of gum disease.
Recognizing the symptoms of gingivitis early and seeking prompt dental intervention is crucial. Symptoms such as persistent bad breath, gum redness, swelling, and bleeding during brushing or flossing should not be ignored. These are clear signals that your gums require attention to prevent the escalation of periodontal disease. Regular dental check-ups allow for early detection and treatment, significantly reducing the risk of advancing to more severe stages of periodontal disease.
What is the Best Toothpaste for Periodontal Disease?
Selecting the appropriate toothpaste is a key component in managing and preventing the progression of periodontal disease. For individuals dealing with this condition, the choice of toothpaste can significantly influence the effectiveness of their oral hygiene routine.
Toothpastes formulated with active ingredients such as stannous fluoride and triclosan are particularly beneficial for individuals with periodontal disease. Stannous fluoride is known for its ability to strengthen tooth enamel and reduce the occurrence of tooth decay, while also possessing antimicrobial properties that combat the bacteria responsible for gum disease. Triclosan, on the other hand, adds an extra layer of protection by effectively reducing bacterial infection and controlling plaque accumulation.
In addition to these ingredients, looking for toothpastes specifically branded as anti-gingivitis or anti-plaque can also provide targeted benefits for those with periodontal concerns. These formulations are designed to not only clean teeth but also to address the root causes of gum disease by reducing plaque build-up and inflammation in the gums.
Moreover, the presence of the American Dental Association (ADA) Seal of Acceptance on toothpaste packaging is a key indicator of its quality and effectiveness. This seal signifies that the toothpaste has undergone rigorous testing and meets the stringent standards set by the ADA for safety and efficacy in oral care.
For those with sensitive gums or advanced periodontal disease, toothpastes with gentle formulations that include aloe vera or other soothing agents can be advantageous. These ingredients can help to alleviate gum irritation while still providing the necessary plaque control.
Ultimately, while the right toothpaste can play a critical role in managing periodontal disease, it should be part of a comprehensive oral health regimen. Regular brushing and flossing, combined with professional dental cleanings and check-ups, are essential to keeping periodontal disease in check and maintaining overall oral health.
What Happens if Periodontal Disease Goes Untreated?
Ignoring periodontal disease is a gamble with high stakes for one's oral and overall health. When left untreated, periodontal disease can escalate from the mild inflammation of gingivitis to the more severe condition known as periodontitis. This advanced stage of gum disease is not just a dental concern but a systemic health issue.
In periodontitis, the inflammation penetrates deeper, affecting not only the gums but also the bone structure that supports the teeth. This progression leads to the formation of pockets between the gums and teeth, which become breeding grounds for harmful bacteria. These pockets deepen over time, further complicating cleaning efforts and exacerbating the bacterial infection.
As the disease advances, the support structures, including the jawbone and connective tissues that hold the teeth in place, begin to deteriorate. This breakdown results in the loosening of teeth, which can lead to their eventual loss if the disease remains unchecked. The loss of teeth not only affects one's ability to chew and speak but also has significant implications for facial aesthetics and self-confidence.
The ramifications of untreated periodontal disease extend beyond the mouth. Research has established connections between periodontal disease and various systemic health issues. The bacteria responsible for periodontal disease can enter the bloodstream through the gum tissues, potentially affecting distant organs and systems.
For instance, there is a well-documented link between periodontal disease and cardiovascular health. The inflammation caused by the bacteria can contribute to the buildup of plaques in the arteries, leading to an increased risk of heart disease and stroke. Similarly, in individuals with diabetes, periodontal disease can exacerbate blood sugar control issues, leading to a vicious cycle where each condition worsens the other.
Respiratory health can also be compromised as bacteria from infected gums are inhaled into the lungs, potentially causing respiratory conditions like pneumonia. Additionally, periodontal disease has been associated with rheumatoid arthritis, with studies suggesting that the inflammation in the gums can exacerbate the inflammation in the joints.
Pregnant women with periodontal disease face additional risks, including preterm birth and low birth weight babies. The inflammatory response triggered by the gum infection is thought to influence these adverse pregnancy outcomes.
Periodontal disease, while common, is preventable and manageable with the right care and early intervention. If you're experiencing symptoms like red, swollen gums, or if it's been a while since your last dental check-up, don't wait. Schedule an appointment with our office today to ensure your gums and overall health are in optimal condition. Let's work together to keep your smile healthy and bright!