Specialty Dentistry
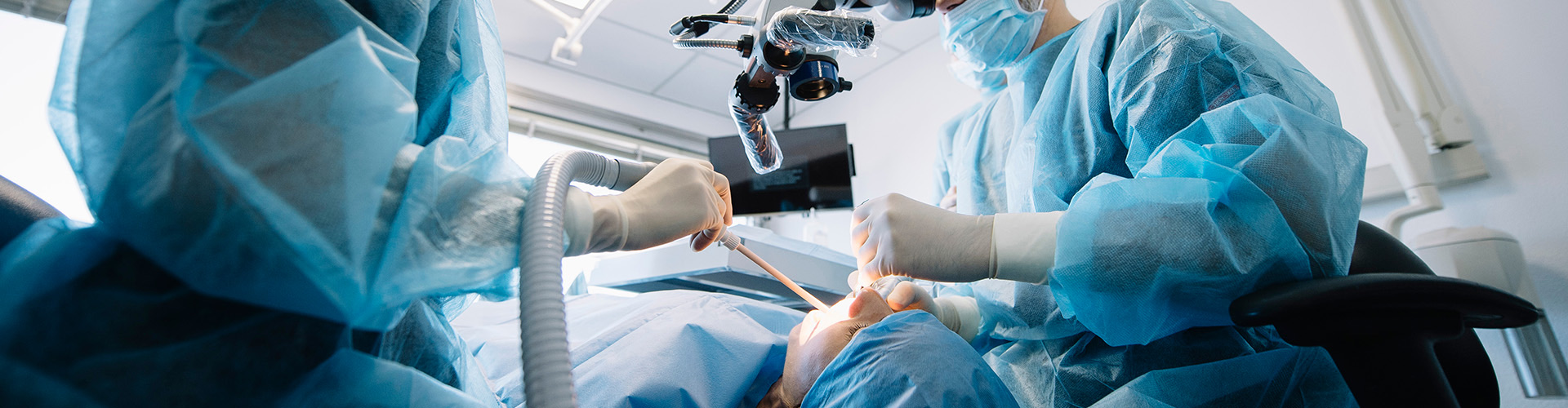
Demystifying Craniofacial Surgery: What You Need to Know Before Your Appointment
For many, the world of dental care extends no further than cleanings and fillings. However, the realm of craniofacial surgery delves deep, addressing problems that extend beyond the realm of basic dental care. Whether you're a patient curious about the process or someone simply seeking more knowledge, this blog aims to clarify the intricacies of craniofacial surgery.
And, if by the end you feel you're in need of a consultation, our clinic is here to help!
How do you prepare for oral surgery?
Oral surgery is a significant event in anyone's healthcare journey. While the idea might seem daunting, thorough preparation can make the experience much smoother. Below, we delve deeper into the necessary steps for ensuring you're ready mentally, physically, and logistically.
Consultation – The Foundation of Understanding:
Your initial consultation isn't just a formality; it's a golden opportunity. It allows you to grasp the specifics of your procedure. Use this time to discuss any medical conditions or medications you're currently on. Your oral surgeon should be aware of these details to ensure the surgery's safety and success. Moreover, never hesitate to ask questions. The more you understand about what's going to happen, the less anxious you'll feel.
Food & Drink – The Art of Fasting:
The instructions you'll receive about fasting largely depend on the kind of anesthesia you'll be given. As a general rule, it's often recommended to abstain from solid foods for at least 8 hours before the procedure. However, this doesn't mean you should be dehydrated. Drinking clear liquids, unless otherwise instructed, can be done up until a few hours prior to the surgery.
Travel – Safety Above All:
Post-surgery drowsiness is a common side effect, especially if general anesthesia or certain sedatives are used. Therefore, driving yourself home isn't just risky; it's potentially dangerous. Plan ahead: whether it means asking a friend or family member to accompany you, or scheduling a cab or ride-share service. The key is to ensure you have a safe way to get home without having to navigate traffic in a postoperative state.
Setting Up for Recovery – Your Comfort Zone:
Once the surgery is done, your comfort during recovery plays a crucial role in how quickly and smoothly you heal. A few preparations can make a world of difference:
- Food: Stock up on soft foods like soups, yogurt, and mashed potatoes. These will be easier on your surgical site and require less effort to consume.
- Resting Area: Ensure your resting space, whether it's a bed or couch, is equipped with essentials like water, medications, a phone, and maybe a good book or TV remote.
Post-op Expectations – Navigating the Aftermath:
After the surgery, it's essential to know what to expect. Your surgeon will provide guidelines tailored to your specific procedure, but a few general rules apply:
- Downtime: The recovery period varies based on the procedure. Always ensure you've given yourself enough time to heal before jumping back into daily activities.
- Dietary Shifts: In the days following the surgery, your diet will likely need to change. Hard or spicy foods might need to be avoided, while cold items might offer relief.
- Medication Adherence: Stick to the medications prescribed. They help manage pain and fend off potential infections. Always check with your surgeon before taking any additional medicines, even over-the-counter ones.
Remember, preparation is more than half the battle. With the right steps, you'll be setting yourself up for a seamless surgical experience and a swift recovery.
Do I have to be referred to an oral surgeon?
Not necessarily! While many patients are referred by their dentist, it's also common for patients to approach an oral surgeon directly, especially if they're aware of their surgical needs.
Recognizing the Need:
It's essential to recognize when professional help is needed. Conditions like impacted wisdom teeth, jaw joint issues, or facial pain might necessitate a visit.
Is oral surgery covered by medical or dental insurance?
The intricate world of insurance can sometimes feel like a maze, especially when it comes to discerning what is covered and what isn’t. Oral surgery, in particular, finds itself nestled in a gray area of this labyrinth. On one hand, there are surgeries that are predominantly dental in nature – think wisdom tooth extractions or dental implant placements. These procedures typically fall under dental insurance. However, on the flip side, we have surgeries that intertwine with broader medical issues. For instance, a surgery required due to facial trauma from an accident or procedures linked to congenital anomalies often falls under the purview of medical insurance.
Navigating this dichotomy isn't just about understanding the type of surgery but being proactive in ensuring that you aren’t caught off guard financially. A crucial step here is open communication with your insurance provider. Before you even set a date for your surgery, it's wise to get on a call or arrange a meeting with them. Seek explicit information about what procedures are covered, to what extent, and under which branch of insurance. This preemptive clarity can save a lot of post-operative financial stress.
But that's not the only conversation you should be having. Your oral surgeon’s office, given their experience with numerous patients, often has a clear understanding of the financial logistics involved. They can provide you with a detailed breakdown of the costs associated with your surgery. This itemized list doesn't just help you plan your finances but can be an invaluable asset when filing insurance claims or when discussing coverage with your insurance provider.
In conclusion, the overlap between medical and dental insurance when it comes to oral surgery requires a bit of legwork on your part. Being proactive, asking the right questions, and ensuring open lines of communication with both your insurer and your surgeon's office are pivotal steps in ensuring you’re adequately covered and prepared.
What's the difference between an oral surgeon and a dentist?
The realm of oral healthcare is vast, and within it, different professionals have specialized roles to play. One of the most common queries is the distinction between an oral surgeon and a general dentist. It's a distinction that lies primarily in education, training, and the scope of their respective practices.
Education and Training:
All journeys in oral healthcare begin at dental school, a rigorous program that equips aspirants with the foundational knowledge and skills required to care for our teeth and gums. However, oral surgeons don't stop there. Post dental school, they dedicate an additional 4-6 years of their lives for specialized surgical training. This further education enables them to administer various types of anesthesia and perform a broader range of complex surgical procedures.
Scope of Work:
When we think of a dentist, we often visualize the friendly face we visit for our bi-annual cleanings, the occasional cavity filling, crafting crowns, or perhaps even designing a set of braces for aligned teeth. Their realm largely revolves around preventive care and general oral health maintenance.
On the other hand, oral surgeons are the specialists we turn to when we encounter more intricate challenges. They deal with complicated tooth extractions (like impacted wisdom teeth), corrective jaw surgeries, certain facial injury treatments, and sometimes even delve into cosmetic surgical procedures that go beyond the scope of a typical dentist.
Recovery and Care Post-surgery:
The aftermath of any surgical procedure is as critical as the procedure itself. While the specifics of post-operative care depend on the type of surgery, a few universals apply:
Medication is often prescribed post-surgery to help manage pain and keep potential infections at bay. Adhering to this prescribed routine is paramount for a smooth recovery.
Oral hygiene can't take a back seat even after a surgery. Gentle brushing, avoiding the surgical site initially, and using prescribed mouthwashes can keep complications at bay.
Being observant can make a difference. While some discomfort post-surgery is expected, certain symptoms like uncontrolled bleeding, excessive swelling, or unusually intense pain signal that something might be amiss. In such cases, it's crucial to contact your oral surgeon promptly.
In Conclusion:
The world of craniofacial surgery might initially seem like uncharted territory, filled with medical jargon and unfamiliar procedures. However, with a deeper understanding and the expertise of a seasoned surgeon, the path becomes clearer and less intimidating. Our clinic stands ready to offer guidance, support, and expert care at every juncture of this journey.
Considering craniofacial surgery for yourself or a loved one? We invite you to schedule a consultation with our clinic, where we aim to address all your concerns and guide you towards the best possible outcome.